Published 27 April 2021
Increasing Covid-19 infections in many countries are renewing concerns about the manufacturing and distribution of vaccines. In recent months, many vaccine-producing countries have tightened rules for exporting vaccines and their ingredients. What’s receiving far less attention are the incentives critical to manufacturers. Improving incentives and de-risking investments are important in encouraging more vaccine production.
According to the World Health Organization, reported Covid-19 infections are increasing around the world except in some parts of Europe and Africa. The persistence of the virus and its variants has led to policy responses that are concerning for global trade. In recent months, many vaccine-producing countries have tightened rules for exporting vaccines and related ingredients. Meanwhile, a growing number of voices are urging vaccine developers to share their intellectual property so that others can start manufacturing.
What is receiving far less attention are the incentives critical to vaccine manufacturers. Improving incentives for manufacturing and de-risking investments would help manufacturers ramp up production and shift the focus of conversation from scarcity to sufficiency. During a global pandemic, the costs of doing too much are less than the costs of doing too little.
When considering the scaling up of production capacity, manufacturers must weigh the pros and cons of expansion. While discussions of pharmaceutical supply are often polarized, a balanced approach requires recognition of both global health imperatives and incentivizes for companies to ramp up production. In a recent paper co-written with Bernard Hoekman of the European University Institute, and Michele Ruta and Nadia Rocha of the World Bank Group, these proposed incentives are outlined in greater detail.
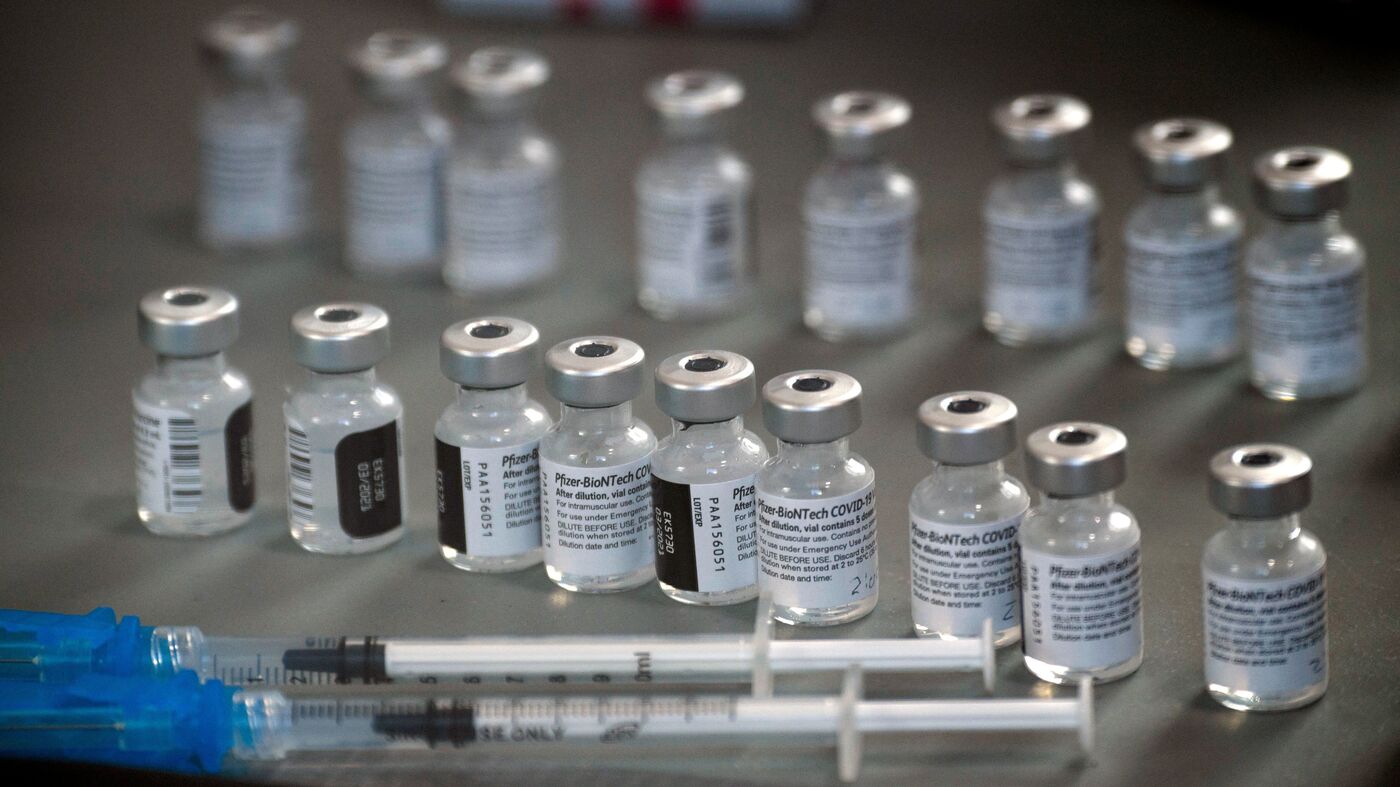
For vaccine manufacturers, any business case must take account of risks that are often as sizeable as the costs of investment. For example, in recent years Pfizer has invested some EUR 500 million in its production facility in Puurs, Belgium. Admittedly, some of this expenditure predates the pandemic and targeted vaccines unrelated to Covid-19. Still, the sums are not a trivial commitment for shareholders.
The second big risk relates to the revenue stream. Often, vaccines are administered as a ‘one-off’ that, once administered, requires no follow up treatment. As a result, the recovery of any production costs and investment must occur during a relatively short period of time. There may be other payoffs in terms of expertise acquired during vaccine development. However, the revenue stream remains limited.
The third risk is the uncertainty about the possible scale of a pandemic. Manufacturers are concerned that outlays may far exceed total revenues. The H1N1 pandemic in 2009 – 2010 provides a lesson. When the outbreak proved to be less severe than expected, several European governments cancelled their vaccine orders. Those governments were entitled to do so. However, vaccine producers were also entitled to feel dismayed when their revenues fell short of expectations and add risk to the companies’ finances.
The experience was significant for Richard Hatchett, the Chief Executive Officer of the Coalition for Epidemic Preparedness Innovations (CEPI). He described the approach of governments to call (drug manufacturers) during an emergency and, “demand that they do this and that (and) reallocate resources, disrupt their daily operations in order to respond to these events — is completely unsustainable.”
Businesses typically take account of other policy-induced risks. Risk assessments of potential investments will consider if the prospective host government has a track record of nationalist trade policy. Should a government ban vaccine exports, then expected sales revenue from local buyers alone will largely determine the commercial viability of any capacity investment. That presents a disincentive. Another potential worry for investors is the possibility of vital vaccine ingredients also joining the export ban list.
In the case of Covid-19, there are added risks. This is the first time that vaccines were successfully developed using mRNA technology. Given the lack of experience in large scale production of vaccines based on this technology, there are plausible concerns about production delays, quality control, and backlash from governments. All these questions were likely weighed by private sector decision-makers.
Reducing these risks should be a priority. Governments have understood this to some degree, with some public authorities partially financing the building of new facilities. However, more could be done to reduce the risks for producers. The trade policy dimension has been mentioned above. Assuring the availability of key qualified personnel (including through their cross-border movement), as well as internal and cross-border trade facilitation, would also help.
However, the emergence of variants of the original Covid-19 strain may transform the commercial calculus. If Covid-19 and its variants become a recurring problem, then regular “booster” jabs will be needed for much of the world’s adult population.
Instead of being a “one-off” event with a burst of revenue earned for a few years, vaccine development may then evolve into the production and distribution of booster jabs. This would create a multi-year revenue stream that is more likely to support a higher level of R&D and production capacity–just as it has for booster flu jabs.
Funds will need to be raised at the global level to ensure that developing countries can gain access to any booster jabs. Such developments can bring together governments, the private sector, and international organizations to develop multi-year cooperation and initiatives that can subsequently boost a collective pandemic response and promote more inclusive vaccine distribution.
What if de-risking creates too much capacity? It is an intriguing question that contrasts the costs of over-expansion with the costs of under-expansion. Weighing the benefits sheds light on the solution’s potential scale.
Suppose that over-expansion results in over-production of 12 billion doses. If each dose costs an estimated USD 20, the resulting “waste” would amount to USD 240 billion.
That sounds like a lot of money. But figures are relative. Compare the hypothetical costs for perspective. The costs of such ‘over-capacity’ are equivalent to approximately 0.25% of world GDP. In short, speedier vaccine rollout would bring forward the global economic bounce back from the USD 6 trillion in lost potential output suffered in 2020.
Given this context, the costs of producing too many vaccines – of producing so-called waste – would simply amount to peanuts.
© The Hinrich Foundation. See our website Terms and conditions for our copyright and reprint policy. All statements of fact and the views, conclusions and recommendations expressed in this publication are the sole responsibility of the author(s).